
HOME | PRIORITIES & INDICATORS | EDUCATION | SAFETY | MENTAL HEALTH | POPULATION | ECONOMICS | HEALTH | WHERE DO WE GO FROM HERE | SOURCES
Mental Health
Lubbock Area United Way Priority #3: To provide access to all persons in need of mental health services.
Lubbock Area Comprehensive Mental Health Needs Assessment
From December 2018 - July 2019, The Meadows Mental Health Policy Institute (MMHPI) conducted a comprehensive assessment of Lubbock’s mental health needs – and its capacity to meet them. With the support of the City of Lubbock, the Community Foundation of West Texas, Covenant Health System, Lubbock County, StarCare Specialty Health System, Texas Tech University Health Sciences Center, and University Medical Center, they conducted research, provided a detailed overview of their findings (both good and bad), and gave recommendations as to the direction the Lubbock community needs to go in terms of improving mental health services for its citizens.
While the full results are still being evaluated, initial findings include:
-
Lubbock County has 21 psychiatrists, or 6.9 per 100,000 residents, approximately one half the national average.
-
There are no intensive outpatient treatment or partial hospitalization programs available to people with commercial insurance.
-
There is no first episode psychosis (FEP) program to identify and treat people experiencing a psychotic disorder at the earliest possible point – an important gap, especially in a community with a large college-age population.
-
“Lubbock leaders from every sector are committed to fundamentally improving mental health care in their communities and, for at least two years, have engaged in ongoing discussions about strategies to make these improvements. Elected officials, public health officials, philanthropic organizations, the heads of major health systems, law enforcement leadership, academic leaders, social service providers, school districts, and others expressed a deep-seated desire to improve care for people with mental illnesses. This cooperation among leaders is the most critical asset Lubbock has going forward.”
As the full results are reviewed, it will be even more crucial for local stakeholders to collaborate and address the many mental health gaps currently existing on the South Plains. With estimates suggesting only half of people with mental illnesses receive treatment, it is more crucial that access to services for those in need are readily available.
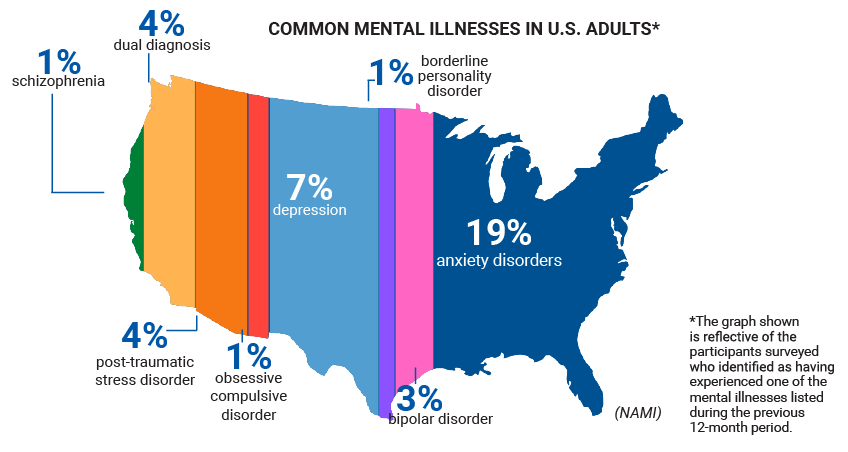
Youth & Mental Health
“The latest CDC data show that the U.S. life expectancy has declined over the past few years. Tragically, this troubling trend is largely driven by deaths from drug overdose and suicide.” (CDC) During this increase, youth suicides (those less than 25 years old) have also risen. (DSHS)
Mental health conditions are very common among teens and young adults. Staff at the Lubbock County Juvenile Justice Center (LCJJC) identified mental health as the most significant challenge for children in the juvenile justice system. It is estimated that 70% of kids in the juvenile-justice system suffer from a serious mental health disorder. (NAMI) However, all 326 people age 0-17 years who were admitted to inpatient care were hospitalized outside of the Lubbock County area due to a lack of local treatment centers. This could potentially lead to additional trauma by moving a child in need away from any local support system.

Adverse Childhood Experiences (ACES)
Issues such as child abuse or neglect, sex trafficking, domestic violence are all traumatic experiences that impact the victim for the rest of their lives. Trauma can change the make-up of your brain which makes preventing early trauma key to improving adult health. “Adverse Childhood Experiences (ACEs) are potentially traumatic events that occur in childhood. ACEs can include violence, abuse, and growing up in a family with mental health or substance use problems. Toxic stress from ACEs can change brain development and affect how the body responds to stress. ACEs are linked to chronic health problems, mental illness, and substance misuse in adulthood.” (CDC)
Preventing ACEs and early trauma is a potential key to helping children and adults thrive. Exposure to ACEs is associated with increased risk for health problems across a lifetime. Yet initial studies showed 61% of adults had at least one ACE and 16% had 4 or more types of ACEs.

Family Counseling Services
Family Counseling Services (FCS) provides individual counseling in the areas of mental health, substance abuse, and victims of sex trafficking. They also provide group therapy services for substance abuse, domestic violence, life skills, parenting, and anger management.
COVID-19 put many of our neighbors at-risk for an increase in stress, anxiety, and other mental health issues. To adapt and continue meeting the needs of clients across the South Plains, FCS was able to switch to a telemedicine format. In 2019, FCS assisted 1,300 individuals through counseling services. While their current numbers are on track with last year, they are seeing a spike in family relationship, substance abuse, and domestic abuse themed sessions largely due to COVID-19.

Loneliness and COVID-19
A recent survey of more than 20,000 American adults found that nearly half report always or sometimes feeling lonely - a situation experts worry could worsen within social-distancing restrictions. Feelings of loneliness can increase risk of depression, anxiety, and are associated with a 26% jump in mortality risk. (TIME)
In addition, a 2017 from the University of Pittsburgh found that people ages 19-23 who spent two hours or more a day on social media were twice as likely to feel isolated as those who spent less time. Another area that may increase due to a spike in social media usage during COVID-19 stay-at-home orders.
